A full migraine attack typically lasts 1 to 2 days, and that recovery window often stretches well beyond the end of the head pain. If you're wiped out after the throbbing stops, that doesn't mean you're weak or overreacting. It means the attack may still be unfolding.
A lot of people expect migraine recovery time to end when the pain ends. But migraine isn't just a bad headache. It's a whole neurological event that can move through stages, change shape, and leave you feeling foggy, sore, shaky, or strangely empty afterward.
If you're reading this while wondering why you still can't think clearly, answer emails, cook dinner, or tolerate bright light, there's a reason. The pain phase may be over, but your brain and body may still be in the postdrome, often called the migraine hangover.
Table of Contents
- Your Migraine Isn't Over When the Pain Stops
- How the timeline works
- The Migraine Attack Timeline at a Glance
- What you can do in each phase
- Why postdrome feels so disruptive
- What postdrome can look like in real life
- Why naming it helps
- What to do during the migraine hangover
- Start with the low-stimulation basics
- Match your support to the symptom that is hanging on
- Medication questions to discuss carefully
- When recovery needs urgent medical attention
Your Migraine Isn't Over When the Pain Stops
You wake up the morning after the pain eases and expect life to click back into place. Instead, your brain feels foggy, your body feels drained, and ordinary tasks seem heavier than they should.
That can be one of the most confusing parts of migraine. The pain phase may be ending, but your nervous system may still be recovering. For many people, the attack is not over until their energy, thinking, and tolerance for light, sound, and activity start to feel more normal again.
Migraine works more like a storm system than a single burst of pain. The headache is the part people can see. The rest of the attack can include warning signs before the pain and a recovery period after it. If you only count the hours your head hurts, you can miss a large part of what your body is dealing with.
That shift in perspective matters.
A headache is one symptom. A migraine attack is a neurological event that can affect mood, attention, digestion, senses, sleep, and energy before, during, and after head pain. So if you still feel slow, weak, or overstimulated once the pain fades, that does not mean you are overreacting or recovering "wrong." It means the attack may still be winding down.
Practical rule: Mark the end of a migraine by the return of function, not pain alone.
This idea can also help you make better choices in the hours after the headache lifts. If your brain is still in recovery, pushing straight back into screens, errands, workouts, or a packed schedule can feel like asking a sprained ankle to sprint. You may do better with a quieter landing. Water, a simple meal, rest, gentle movement, and lower sensory input often fit this stage better than trying to catch up all at once.
It also changes how you track migraine recovery time. Logging only the start and stop of pain gives you part of the timeline. Logging when you could focus again, tolerate noise again, or return to normal activity gives you the part that often matters most in daily life.
The Four Phases of a Migraine Attack
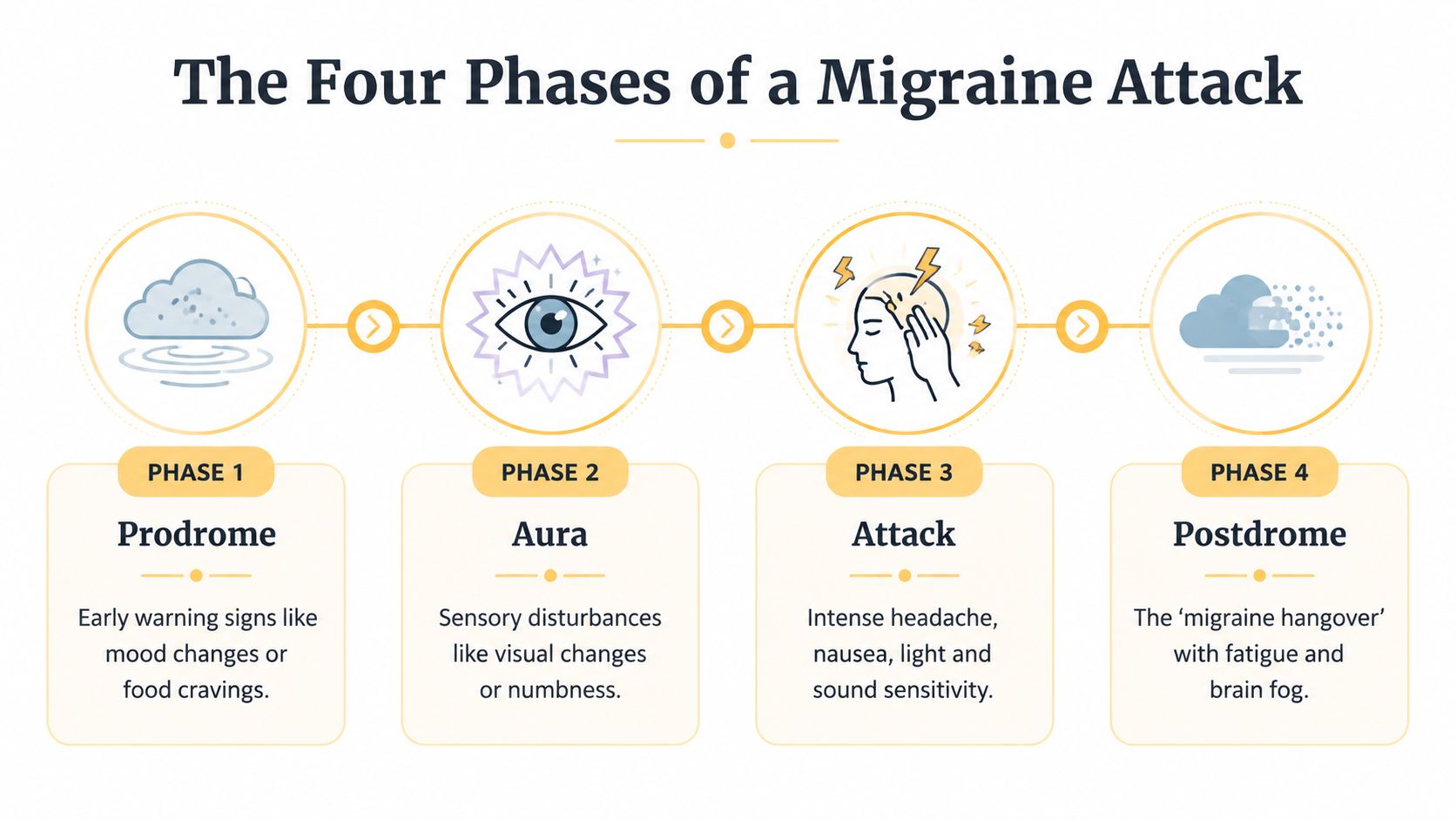
A migraine attack often unfolds in stages, more like a weather pattern than a single hit of pain. You may notice an early shift, then a wave of neurological symptoms, then the headache itself, followed by a drained recovery period. Some people move through all four phases. Others only notice two or three.
How the timeline works
The first phase is prodrome, the warning stage. This can begin before head pain and may show up as fatigue, mood changes, food cravings, neck discomfort, or trouble focusing. Many people describe it as a hard-to-name sense that something is off. If you catch this phase early, you may have more time to protect your energy, adjust your plans, or use the treatments your clinician has recommended.
The second phase is aura. Some people have it. Many never do. Aura includes temporary neurological symptoms such as visual changes, tingling, numbness, or trouble speaking clearly. It can feel alarming if you do not know what it is, which is one reason tracking matters. If aura is part of your pattern, logging what it feels like and how long it lasts can help you respond faster and describe it more clearly to a doctor.
Next comes the headache phase, which is commonly recognized. The pain may throb or pulse and often comes with nausea, light sensitivity, sound sensitivity, or a stronger reaction to smells and movement. Untreated migraine headache can last 4 to 72 hours. During this phase, your goal usually shifts from prevention to reducing input, easing symptoms, and doing less.
The final phase is postdrome, the recovery stage after the main pain lifts. You may feel wrung out, foggy, weak, dizzy, or emotionally flat. For some people, this stage is brief. For others, it stretches into the next day or longer, which is why migraine recovery time can feel much longer than the headache itself.
A migraine works like a storm front, a peak, and the soggy ground left behind.
The Migraine Attack Timeline at a Glance
| Phase | Typical Duration | Common Symptoms |
|---|---|---|
| Prodrome | Varies | Mood changes, fatigue, food cravings, feeling "off" |
| Aura | Varies | Visual changes, tingling, numbness, speech trouble |
| Headache | 4 to 72 hours untreated | Throbbing head pain, nausea, photophobia, phonophobia |
| Postdrome | Varies | Exhaustion, weakness, confusion, dizziness, muscle aches |
What you can do in each phase
The most useful self-care often changes with the phase. Treating the whole attack the same way can make it harder to spot patterns or support your body at the right time.
- During prodrome: Look for your earliest clues. Yawning, irritability, neck stiffness, or sudden cravings can be your version of a warning light on the dashboard. Write down what showed up first, what time it started, and what you were doing that day.
- During aura: Lower stimulation quickly. Dim screens, step away from bright light, and pause tasks that need visual focus or fast decisions. If you have prescribed treatment for this stage, knowing that aura has started can help you use it sooner.
- During the headache phase: Shrink the demand on your brain. Keep the environment quiet, postpone nonurgent choices, and use the comfort measures or medication plan that usually helps you. Tracking what made this phase shorter or harder can be more useful than only tracking pain level.
- During postdrome: Measure recovery by function. Note when you could think clearly, tolerate noise, eat normally, or return to regular activity. Those details show you how long the full attack lasted, not just when the pain stopped.
The Migraine Hangover Deconstructed
You wake up the day after the headache fades, expecting to feel normal again. Instead, your body feels heavy, your thoughts feel slow, and even simple tasks seem to take extra effort. That after-effect has a name. It is called postdrome, and many people describe it as the migraine hangover.

Why postdrome feels so disruptive
Postdrome is the recovery phase after the main pain has eased, but your nervous system has not fully settled yet. The attack is winding down, but your brain and body are still doing cleanup.
That is why the mismatch can feel so confusing. The sharpest symptom, head pain, may be gone, while other symptoms are still interfering with your day.
Common postdrome problems include fatigue, trouble focusing, dizziness, muscle soreness, mental fog, and lingering sensitivity to light or sound. For some people, it feels like recovering from a storm. The thunder has passed, but the ground is still soaked and unstable.
What postdrome can look like in real life
Postdrome often shows up as reduced function more than dramatic pain.
You might answer messages more slowly. Reading may take more effort. A grocery store can feel too bright and too loud. Your body may feel wrung out, almost like you used energy reserves you have not replaced yet.
Some people feel emotionally flat or unusually irritable. Others feel shaky, weak, or slightly off balance. If you have ever thought, "The migraine is over, so why do I still feel awful?" postdrome is often the missing explanation.
Recovery after migraine can look mild from the outside while still limiting how well you can think, move, and tolerate stimulation.
Why naming it helps
A name gives you a clearer way to respond. Instead of judging yourself for being slow or unproductive, you can treat postdrome as a real phase with its own needs.
That shift matters because the best question is not only, "Is the pain gone?" A better question is, "What can I do again without making recovery harder?"
What to do during the migraine hangover
Postdrome care works best when you match it to the symptoms you experience.
If your brain feels foggy, lower the cognitive load. Put off detailed decisions, long meetings, or tasks that need sustained concentration. If light and sound still bother you, keep stimulation low for a little longer instead of forcing a full return to normal. If you feel drained or sore, focus on basics such as fluids, food, rest, and gentle movement if that feels tolerable.
Tracking helps here too. Write down when the pain ended, then note when your thinking cleared, when noise felt manageable, and when you could return to normal activity. That gives you a more accurate picture of your true recovery time. Over several attacks, you may start to see patterns, such as longer postdrome after poor sleep, vomiting, or pushing through work too soon.
Postdrome is not a personal failure to bounce back. It is part of the migraine process, and understanding that can help you plan your recovery with more patience and more control.
What Shortens or Lengthens Your Recovery
Migraine recovery time isn't fixed. Two attacks can look similar at first and leave you with very different aftermaths.
Attack factors
Some recovery periods are longer because the attack itself was more draining. A harder pain phase, strong nausea, vomiting, poor sleep during the attack, or extended light and sound sensitivity can leave you more depleted afterward.
The shape of the attack matters too. If the symptoms build slowly and linger, your body may need more time to settle. If the pain stops but dizziness, weakness, or sensory sensitivity hang on, it may still feel like the migraine is "still there" even though the worst pain has passed.
Your baseline matters too
Your starting point affects recovery. If you're already sleep-deprived, under unusual stress, dehydrated, or trying to function through back-to-back obligations, the same migraine may hit harder on the way out.
Some people also notice that certain migraine types create a different recovery feel. Vestibular migraine, for example, may leave more lingering disequilibrium or motion sensitivity. Chronic migraine can blur the lines between one attack ending and another beginning, making recovery harder to identify.
- Sleep debt: Even one rough night can make your brain less resilient the next day.
- Stress load: A tightly packed schedule can make it harder to rest when your nervous system needs quiet.
- Sensory environment: Bright offices, loud commutes, and long screen sessions can drag recovery out.
- General health context: Neck pain, anxiety, illness, or hormonal shifts may complicate how you recover.
Treatment timing and the recovery ripple effect
The timing of your treatment approach can matter. If you catch an attack early and your symptoms are managed sooner, recovery may feel less jagged. If relief comes late, or if nothing really settles the attack, the postdrome may feel heavier.
This doesn't mean you did anything wrong. Migraine is variable by nature. But it does mean your own records can reveal patterns, especially around sleep, timing, stress, hydration, and what helped you function afterward.
The question isn't only "How bad was the migraine?" It's also "What condition was my body in when it started, and what happened during the hours after?"
How to Support Your Body During Recovery
This article is for informational purposes and is not medical advice. Consult a healthcare provider for personalized guidance.
The pain has eased, but your brain and body may still feel wrung out. Many people expect to bounce back the moment the headache lifts, then feel confused when they are still foggy, shaky, or unusually tired hours later. Recovery often works more like cooling down after a sprint. The hardest part may be over, but your system still needs time to settle.

A good recovery plan matches what your body is asking for in that phase. If your head feels tender and light still hurts, reduce input. If nausea is fading but energy is low, focus on fluids and easy food. If your thoughts are returning but you feel fragile, re-enter the day slowly instead of testing your limits all at once.
Start with the low-stimulation basics
During postdrome, your nervous system may still react as if the volume is turned up too high. Light, noise, screens, strong smells, and mental multitasking can all feel larger than they should. A quieter setting gives your brain fewer signals to sort through while it resets.
Start simple and steady.
- Drink fluids gradually: Small, regular sips are often easier than trying to catch up all at once.
- Eat easy, familiar foods: Toast, rice, soup, crackers, yogurt, or whatever usually sits well for you can be gentler than rich meals.
- Lower sensory load: Dim screens, soften lights, reduce noise, and avoid strong scents if they still bother you.
- Try gentle movement only if it helps: A short walk, light stretching, or slow breathing can help some people feel less stiff or foggy. Rest is a better choice if movement makes symptoms louder.
- Scale back expectations for the day: The end of pain is often the start of recovery, not a signal that your brain is ready for full speed.
This phase-specific approach matters. Recovery support is not one big rule called "rest more." It is a set of small adjustments based on what is still lingering.
If you want more practical migraine education that connects symptoms, triggers, and recovery patterns, the articles on the Relief migraine education blog can help.
Match your support to the symptom that is hanging on
Different post-migraine symptoms call for different kinds of care. Brain fog often responds best to fewer decisions, shorter tasks, and breaks from screens. Fatigue usually calls for food, fluids, and real rest instead of caffeine and pushing through. Neck soreness may improve with a supportive pillow, gentle stretching, or heat if that is something your body tolerates well.
This is less about doing more and more about removing friction.
A useful question is: "What feels overloaded right now?" If the answer is your eyes, dim the room. If it is your stomach, keep food plain. If it is your thinking, postpone anything that needs sharp concentration. That gives you a little more control during a phase that can otherwise feel vague and frustrating.
Medication questions to discuss carefully
Over-the-counter options may be part of some people's migraine plan, but they are not right for everyone, and frequent use can create problems for some patients. If you find yourself needing them often, or if pain treatment helps the headache but leaves you wiped out for a long time afterward, bring that up with a clinician.
Prescription treatment decisions should stay with your healthcare provider. Some people need an acute treatment plan. Some need preventive treatment. Some need both. The right approach depends on your attack pattern, health history, and how much recovery time is affecting daily life.
A short explainer can be useful if you're recovering and want something easier to watch than read:
When recovery needs urgent medical attention
Some symptoms should never be treated as a normal migraine hangover.
Get immediate medical care for a sudden severe headache, headache with fever or stiff neck, new neurological changes, or headache after a head injury.
Also seek urgent care if something feels clearly different from your usual migraine pattern, especially if weakness, confusion, speech trouble, or vision loss is new, severe, or not resolving in the way it normally does.
Track Your Recovery to Understand Your Migraine
If you only track when pain starts and stops, you miss the part that often affects daily life most. Recovery is where you learn how long an attack really costs you.
Write down what happens after the pain lifts. Note when your thinking clears, when your energy returns, whether you still feel dizzy, and what made the day easier or harder. Over time, that record can show whether your migraine recovery time changes with better sleep, earlier intervention, lower stress, or a quieter environment.
What to log after the pain phase
A useful recovery log can be simple.
- End of pain: When the headache eased enough to function at least a little
- End of recovery: When you felt mentally and physically close to baseline again
- Lingering symptoms: Brain fog, fatigue, weakness, dizziness, soreness, light sensitivity
- Helpful supports: Water, food, rest, screen limits, movement, meditation
- Context: Sleep, stress, schedule pressure, travel, weather, hormonal timing
This gives you better language for doctor visits too. Instead of saying, "My migraine lasted a day," you can say, "The pain lasted several hours, but I couldn't think clearly until the next evening."
For people who want a more organized way to spot patterns across symptoms, triggers, and recovery, Relief can support that kind of tracking without turning it into a full-time job.
If you want help noticing your migraine patterns before and after an attack, Relief gives you one place to log symptoms, track recovery, and see the environmental signals that may shape your next migraine day.
Crafted with Outrank app
